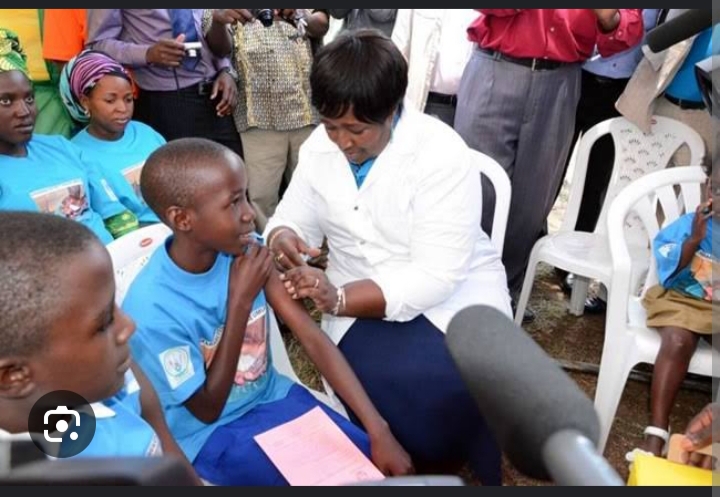
Nakuru County Government, in collaboration with the Ministry of Education and the Teachers Service Commission (TSC), has rolled out a campaign to raise awareness about the Human Papilloma Virus (HPV) and enhance vaccination uptake among 10-year-old girls against HPV, said to be the major cause of cervical cancer.
The County Nursing officer, Wendy Tirop, said at least 5,200 women in the country are diagnosed with cervical cancer annually, with more than 2,000 dying from the disease.
Tirop regretted that women dying from cervical cancer in the county were more than those dying from maternal complications, adding that they were committed to changing the trends through the enhancement of public health services and ensuring that teachers and students are knowledgeable about HPV issues.
She said that the HPV vaccination was most effective when administered to girls before they are sexually active, regretted that signs of apathy towards the HPV vaccine, which have been witnessed in the country, especially among religious leaders, were on the rise, and advised that citizens should be educated on its economic benefits.
“The vaccine targets the HPV subtypes, which are accountable for more than 70 per cent of cervical cancers. Many might not see the immediate effect of the vaccine, so that is why they might procrastinate. We are exploring a number of strategies and creating awareness to make people care about the benefits,” she explained.
Tirop lamented that the HIV agenda had been pushed so much that the country had forgotten about other equally lethal sexually-transmitted viruses such as HPV, a virus she described as a viral infection that spreads through sexual contact and affects both males and females.
The Nursing Officer warned that while HPV infection is cleared away naturally by the immune system of some people, in others the virus could persist and cause cervical cancer within a number of years if no early interventions are taken.
“In HIV-positive women, it takes even less time for the virus to cause cervical cancer. HPV also causes non-cancerous, nipple-like bumps called warts on the skin in the genital area or in other parts of the body, as well as ulcerations. She explained that the ulcerations may make women more vulnerable to other STIs, such as HIV.
She noted that unlike other STIs, HPV infection causes havoc silently, adding that it does not produce any symptoms until in its advanced stages, when it has caused cervical cancer.
Tirop explained that men often carry the virus and transmit it to women during sex, while in men the infection is often linked to penile, anal, and throat cancers, though cases are still rare in Kenya.
The Nursing Officer pointed out that despite the huge dangers posed by HPV, an overwhelming majority of Kenyans remained unaware of the virus and how to protect themselves.
“Not knowing that HPV causes cervical cancer is like not knowing that HIV causes AIDS. Just like HIV testing is done to identify those infected before they progress to the stage of immunodeficiency, so should HPV be tested before women progress to the pre-cancerous and cancer stages, because once identified as positive, someone can be treated,” she explained.
“The fact that less than 5% of women in Kenya know about the link between HPV and Cervical Cancer should be a wake-up call to all stakeholders to raise public awareness so that they can protect themselves,” she added.
Tirop advised Kenyan women to seek regular cervical cancer screening to avoid falling victim to the deadly virus.
According to the World Health Organisation (WHO), the deadly virus, which has no cure yet and is spread through vaginal, oral, and anal sex, has become so common that nearly all sexually active women get it at some point in their lives.
The screening can be done using a Pap smear or Visual Inspection with Acetic Acid (VIA). The two methods check if the virus has caused any abnormal changes in the cervix associated with cervical cancer and give early treatment before it becomes full-blown cancer.
In October 2009, Kenya became the 16th country in Africa to introduce the Human Papilloma Virus (HPV) vaccine into its routine immunisation schedule. This vaccine targeted 800,000 girls aged 10 years.
According to the World Health Organisation, HPV is medically attributed as the most prominent single contributor to cervical cancer.
The virus plays the most central role in the development of this type of cancer. Currently, there are about 100 types of HPV. At least fourteen of these HPV types cause cancer. Two HPV types, known as 16 and 18, cause 70 percent of cervical cancers and lesions.
Cervical cancer is currently ranked as the second-most common cancer among women in the country. It is also ranked as the most common cancer among women aged between 15 and 44 years.
Globally, cervical cancer is the fourth most common cancer in women. In 2018 alone, 18.1 million new cases were diagnosed worldwide, with 9.6 million deaths reported.
The World Health Organisation says that there are three types of HPV vaccines. These include the bivalent, quadrivalent, and nonavalent vaccines.
“All three vaccines are highly efficacious in preventing infection with virus types 16 and 18, which together are responsible for approximately 70 percent of cervical cancer cases globally,” says the WHO.
WHO explains that the quadrivalent vaccine is also highly efficacious in preventing anogenital warts, which is a common genital disease that is almost always caused by infection with HPV types 6 and 11.
“The nonavalent vaccine provides additional protection against HPV types 31, 33, 45, 52, and 58,” states the WHO.
Meanwhile, according to the WHO, HPV vaccination can prevent more than 90 percent of cancers that are caused by HPV infections.
This is echoed by the CDC, which states that with the administration of the HPV vaccine, infections that cause most HPV cancers and genital warts drop by as much as 88 percent among teenage girls and 81 percent among young adult women.
By Esther Mwangi and Samuel Karanja