In March this year, the government appealed to the public for the return of over 20,000 oxygen gas cylinders being hoarded at homes. The appeal came in the wake of alarming reports that health facilities with covid-19 patients were running out of oxygen due to lack of cylinders. Oxygen is a key component in treating moderate to severe cases of Covid-19.
The Ministry of Health notes that daily oxygen demand in hospitals has been on an upward spiral since the coronavirus outbreak in the country. Early last year, daily oxygen demand in hospitals was at 410 tons. By January 2021, the demand had shot to 560 tons. By March, daily demand had surged to 880 tons. There is trepidation that this demand will rise higher and therefore a need of having a robust system in place to address the challenge of oxygen shortages in the country.
To manage such risks, the Health ministry has introduced a policy that puts provision for piped oxygen as a mandatory requirement before approval of all construction plans for health facilities across Kenya.
Cabinet Secretary (CS) for Health Mutahi Kagwe was categorical: No construction plans for health facilities in the country will be approved without incorporating the component of piped oxygen in the plans.
This policy will be adopted as part of a long-term plan to effectively manage sudden widespread surge of Covid-19 through maximisation of oxygen use by patients in need of supplemental oxygen and cushion the healthcare system against being overwhelmed.
“We are moving away from having a single patient-single cylinder scenario. With a piped system, a single cylinder can serve several patients. This is a more effective and safer way and therefore piped oxygen must be a requirement for hospitals,” he said.
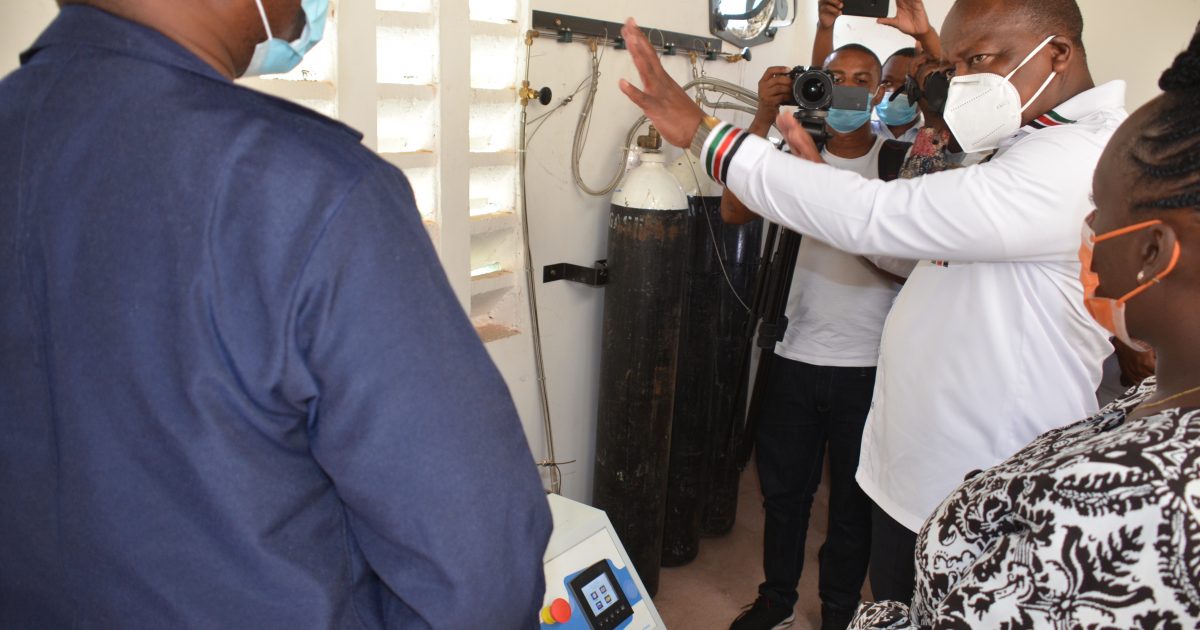
The CS was speaking after touring an oxygen generating plant at Moi County Referral Hospital in Voi. The hospital has already installed a piped oxygen system in two wards and is already in use by patients.
The piped-oxygen requirement is viewed as a precautionary measure to address a scenario where the country might find herself with a huge number of patients requiring oxygen. With almost 40 per cent of the country’s 50,000 oxygen cylinders being kept at homes, the threat of hospitals running out of oxygen looms large.
In countries that have suffered a sharp surge of covid-19 infections, oxygen has been a most-sought after commodity for hospitals. From Italy to India, heart-wrenching scenes of patients in hospital beds with nasal cannulas stuck on their nostrils and others with oxygen masks have become too common.
That such countries with their significantly robust health systems could eventually be overwhelmed by the large number of patients is a sobering reminder of Kenya’s precarious situation.
Even as the policy is being implemented, the CS called out to the counties to make plans for tackling covid-19 with the worst-case scenario in mind. He explained that essential supplies like oxygen, drugs and beds should be factored in with anticipation of the worst that can happen.
“Your planning for Covid-19 in hospitals should have the worst-case scenario in mind,” said the CS.
The worst-case scenario implies the measures that hospitals can tap to for management and treatment of unprecedented surge in covid-19 infections. Kenya has a current positivity rate of sub-10 per cent with an average daily infection of around hundreds.
Still, this rate is considered alarmingly high according to Kenya’s infection standards. However, government interventions including lockdowns, wearing of masks and banning of crowds have given hospitals ability to manage their cases. Even when bed capacities in some hospitals were reportedly full, there were available beds in other facilities.
However, the unfolding nightmare in countries like India is a terrifying reminder of the capricious nature of Covid-19 and its infections patterns. This means a country can move from hundreds of infections daily to hundreds of thousands within weeks.
With such a view in mind, the government has ramped up efforts to strengthen the health system in the counties. This involves enhancing the Oxygen Manufacturing capacity for hospitals. Already, the ministry and development partners have identified 86 health facilities in 30 counties for this initiative. USAID will support five hospitals.
Moi County Referral Hospital in Voi is one of the facilities that will benefit from the government and donor support to increase the oxygen generating and distribution capabilities. Moi Teaching and Referral Hospital in Eldoret has already established the largest oxygen plant in East and Central Africa with a production capacity of 2,000 liters per minute.
“This is the progress we are making. We will eventually need all hospitals to have capacities to handle serious cases but we will start with the ones identified,” he said.
To date, the ministry has disbursed monetary support amounting to Sh 28.8 billion to counties for management of Covid-19. There has also been support in provision of PPEs and hospital equipment.
According to the ministry, the final goal is to have all counties being oxygen-self-sufficient. However, it is not oxygen alone. The government is also working on locally manufacturing Covid-19 vaccine and other essential drugs to cut off dependency on foreign help.
The CS said relying on donors and external sources remained unreliable as such arrangements were prone to abrupt changes in scheduling. He said the county will start procuring the vaccines in bulk and bottle locally. Uganda is one of the countries in East Africa that manufactures ARV for use by AIDS patients.
“We hope to be self-sufficient and produce our vaccines locally,” he said.
The risk of relying on donors for help has become clear after India stopped exporting AstraZeneca vaccines to other countries.
Dr Willis Akhwale, national chair of Vaccine Taskforce, said despite the stoppage, another AstraZeneca consignment for the second jab, is expected to arrive next month. He however said the eight-week gap between the first and second jab had been increased to 12-weeks.
“We will receive our consignment as planned earlier. The shift from 8 weeks to 12 weeks will not have any adverse health effect,” he said.
The government has ordered alternative vaccines including Pfizer, which will only require a single dose, and Johnson Johnson, which will require two jabs with a window period of three weeks between them.
The government has also ruled out mixing of vaccines stating that all people will be subjected to uniformity in vaccination regimes.
By Wagema Mwangi